NexCAR19™ is for patients with challenging B-cell cancers, which are often inadequate to treat with chemoimmunotherapy.
NexCAR19™
A New Hope for Hard to Treat B-Cell Cancers
An Overview of NexCAR19™
A breakthrough in precision oncology, NexCAR19™ (Talicabtagene autoleucel) is a second-generation, autologous, CD19-directed chimeric antigen receptor (CAR) T-cell immunotherapy. Built on a fully humanized molecular platform, it is precision-engineered to address the critical unmet need in relapsed or refractory B-cell malignancies.
NexCAR19™ is a prescription therapy indicated for specific relapsed or refractory B-cell Non-Hodgkin’s Lymphomas and B-cell Acute Lymphoblastic Leukaemia in patients whose frontline or other standard treatments have been unsuccessful.
Response Rate
Response Rate
Longest Remission
Success Rate
Turnaround
Which cancers can NexCAR19™ treat?
Unmet Needs in Relapsed/Refractory B-Cell Malignancies
Transforming outcomes for patients with relapsed/refractory B-cell malignancies—where current treatments fall short
~100,000
Annual Estimated Diagnosed Cases of B-ALL & DLBCL in India
~40%
Relapses in patients with DLBCL, of which 10% have refractory disease
> 60%
Patients requiring a Stem Cell Transplant are unable to receive one.
~41%
Historical survival rate in patients with B-ALL
Patient Journey Overview
Step 1: Eligibility Assessment
Determine Suitability for NexCAR19 Therapy
Evaluate the patient against NexCAR19’s eligibility criteria, including diagnosis, disease status, prior lines of therapy, and performance status.
Step 2: Slot Scheduling
Coordinate Leukapheresis Timing Based on Clinical Readiness
Once eligibility is confirmed, our team will contact you to schedule a leukapheresis slot at your facility or designated center.
Please ensure:
-
Patient is clinically stable and fit for leukapheresis
-
Appropriate drug washout periods are observed
-
Any bridging therapy is planned with manufacturing timelines in mind
Step 3: LSM Collection
Timely & Controlled Pickup of Leukapheresis Material
Upon successful leukapheresis:
-
ImmunoACT or its certified logistics partner will coordinate fresh refrigerated pickup of the Leukapheresis Starting Material (LSM)
-
Ensuring correct labeling, documentation, and chain-of-custody protocols are followed
Step 4: Manufacturing
Stay Informed at Key Checkpoints During Manufacturing
You will receive notifications at the following stages:
-
LSM acceptance and initiation of manufacturing
-
Completion of in-process and final quality checks
-
Expected product readiness and dispatch timeline
Step 5: Infusion & Monitoring
Product Delivery, Infusion Scheduling, and Post-Infusion Care
NexCAR19 will be delivered in advance of your selected infusion window:
-
Confirm patient’s fitness for lymphodepletion and infusion
-
Administer NexCAR19 as per prescribing information
-
Follow structured monitoring protocol post-infusion, including CRS/ICANS management if needed
What are the Side Effects of NexCAR19?
NexCAR19™ may cause side effects that are severe and/or life-threatening.








Unmet Needs in Relapsed/Refractory B-Cell Malignancies
Transforming outcomes for patients with relapsed/refractory B-cell malignancies—where current treatments fall short
~100,000
Annual Estimated Diagnosed Cases of B-ALL & DLBCL in India
~40%
Relapses in patients with DLBCL, of which 10% have refractory disease
> 60%
Patients requiring a Stem Cell Transplant are unable to receive one.
~41%
Historical survival rate in patients with B-ALL
Consider NexCAR19™ as a treatment option
The administration of NexCAR19™ (Talicabtagene autoleucel) should be preceded by a thorough clinical risk evaluation and mitigation process at the treatment center. ImmunoACT recommends the following parameters as prerequisites for consideration of NexCAR19 for your patient. These parameters may be required by your patient’s insurer or payer towards their access to CAR-T cell therapy.
B-cell Non-Hodgkin’s Lymphomas (B-NHL)
- Diffuse Large B-cell Lymphoma
- High-grade B-cell Lymphoma, not otherwise specified
- Primary Mediastinal Large B-cell Lymphoma
- Follicular Lymphoma
- Transformed Follicular Lymphoma (tFL)
- Mantle Cell Lymphoma (specify pleomorphic or blastoid)
Confirmed by Immunohistochemistry & Histopathology/Biopsy Reports
B-cell Acute Lymphoblastic Leukaemia (B-ALL)
- Ph+ve B-ALL or Ph-like B-ALL or Not Otherwise Specified
- CD19+ve expression (dim/moderate/bright) on the malignant clone, and absence of a CD19-ve malignant clone
Confirmed by Bone Marrow Aspiration and Biopsy through Flow Cytometry / Immunophenotyping
Approved in patients aged 15 and above, for the treatment of relapsed/refractory B-cell lymphoma and B-cell acute lymphoblastic leukaemia in India
NexCAR19™ was assessed in an open-label, multicentre, phase 1/2 study in six tertiary cancer centres across India. Of 64 patients aged 15 and above with either relapsed/refractor B-cell lymphoma or B-cell acute lymphoblastic leukaemia, 14 were enrolled in Phase 1, and 50 were enrolled in Phase 2. At an efficacy dose of at least 5 × 10⁶ CAR T cells per kg, NexCAR19 demonstrated an overall response rate of 73%. The trial exhibited a manageable safety profile with high efficacy in a difficult-to-treat population with B-cell malignancies, with these results published in Lancet Haematology
Recommended Pointers for Eligibility
- ECOG: 0–2
- Ejection Fraction (EF) on 2D Echo ≥ 45%
- Peripheral Blood ALC ≥ 500/μL or Absolute CD3+ T cell count ≥ 150/μL
- AST/ALT ≤ 3× ULN, Total Bilirubin ≤ 2× ULN (Child-Pugh A/B unless derangement due to malignancy)
- Creatinine Clearance ≥ 30 mL/min
- Well-preserved lung function
- Well-controlled pre-existing medical & surgical comorbidities
- Absence of active infection or acute inflammation
- CNS disease well-mitigated (if involved)
- Viral Marker Negative Status: HIV, HBV, HCV, CMV
📋 B-ALL Specific Criteria
-
Low percentage of blasts in:
-
Peripheral blood
-
Bone marrow
-
-
Presence or absence of extramedullary disease
📋 B-NHL Specific Criteria
-
Low disease bulk:
-
Subjective quantification by nodal size & extent of nodal/extranodal involvement
-
Or metabolically active tumor volume
-
-
LDH levels may be used as additional supporting marker
How does NexCAR19™ work?
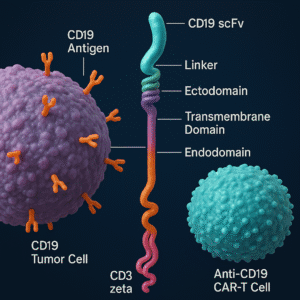
NexCAR19™ utilizes precisely engineered Chimeric Antigen Receptors featuring:
- A humanized single-chain variable fragment (ScFv) antibody that specifically targets CD19 markers found on B-cells
- An optimized flexible spacer that enhances target binding efficiency and cellular interaction
- A specialized 4-1BB co-stimulatory domain that significantly boosts T-cell activation, promotes robust proliferation, and supports long-term persistence
- CD3ζ signaling components that trigger potent T-cell immune responses upon cancer cell recognition
Proven Clinical Performance
Our anti-CD19 binding technology has demonstrated remarkable persistence in clinical settings, with documented durability of action extending beyond 24 months in select patients. The humanized ScFv component delivers exceptional efficacy while contributing to a reduced incidence of severe treatment-related toxicities.
Superior Therapeutic Profile
NexCAR19™ modified T-cells offer a comprehensive treatment solution:
- Safety: Rigorously tested cellular product with established safety profile
- Durability: Long-lasting anti-cancer activity for sustained disease control
- Effectiveness: Consistent response rates across diverse patient populations
Optimized Dosing Strategy
With an efficacy threshold of more than 5 million CAR-T cells per kilogram of body weight, NexCAR19™ achieves exceptional tumor penetration and maintains effectiveness even in challenging high-risk patient populations.
NexCAR19™ is a type of CAR-T cell therapy. T-cells are naturally made by your body as an advanced defense against viruses and cancer cells. As they mature, they develop specific connectors (receptors) to target key signals in cancer cells. However, cancers can escape the inbuilt defense mechanism of T-cells, which can lead to an increase in tumor burden and can result in the survival of cancer cells and a further increase in tumor burden. CD19 is a protein commonly present on the surfaces of certain B-cell cancers.
Our scientists have designed instructions for your T-cells to express unique proteins called Chimeric Antigen Receptors (CARs) on their surface, which will enable them to bind to a specific target on the cancer cells. These instructions are delivered genetically using a vehicle known as a lentiviral vector.NexCAR19 targets a marker called CD19, which is commonly present on the surface of cancerous B-cells.
1. Isolate
Select and activate T-cells from the patient’s blood sample.
2. Program
Deliver genetic instructions to T-cells using viral vectors.
3. Engineer
Enable T-cells to express Chimeric Antigen Receptors (CARs).
4. Expand
Multiply CAR-T cells to achieve the therapeutic dose.
5. Infuse
Administer CAR-T cells to the patient for targeted cancer treatment.
Smarter CAR-Construct & Design for Safer Treatment
At the heart of ImmunoACT’s innovation is a next-generation cell and gene therapy platform, purpose-built to deliver affordable efficacy without compromising safety. Our approach blends cutting-edge science with thoughtful design to make these therapies more accessible and tolerable.
Our CAR-T constructs use fully humanized components, making them more “familiar” to the immune system. This reduces the risk of rejection, minimizes off-target toxicity, and improves patient experience by lowering the need for intensive supportive care.
Each CAR we design includes:
- A single-chain variable fragment (scFv) tailored for precise tumor targeting
- A flexible hinge (spacer) to enable optimal antigen engagement
- A CD8α transmembrane domain for enhanced stability
- A 4-1BB co-stimulatory domain to support T-cell survival and sustained action
- A CD3ζ signaling domain to trigger strong and specific immune responses
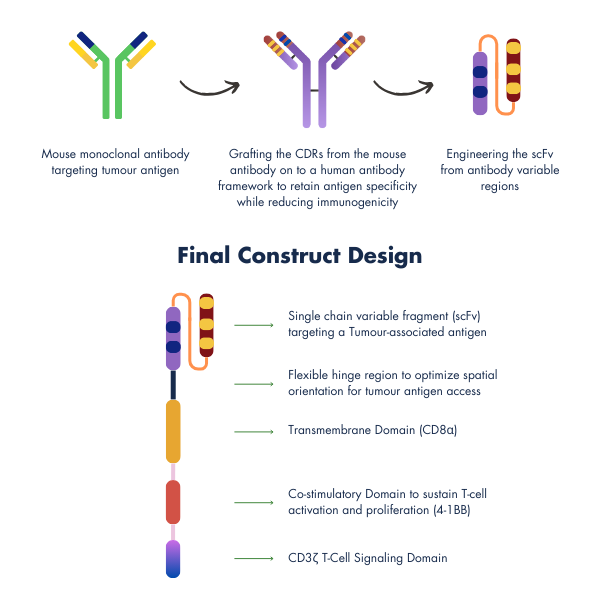
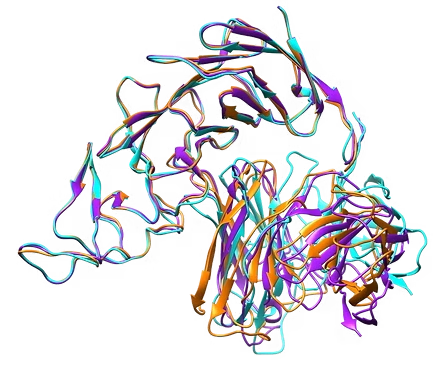
Our CAR-T therapies integrate humanized sequences and undergo rigorous optimization to ensure potency, persistence, and safety. By reducing the likelihood of severe toxicities, we are not just improving patient safety, we are redefining how cell therapies can be delivered.
The gene sequence of the CAR construct is first integrated into a plasmid, which is then used to produce a lentiviral vector. This vector delivers the CAR gene into T cells, enabling them to recognize and attack cancer cells.
NexCAR19™ Manufacturing Process
1. Leukapheresis
This forms the foundational starting material for autologous CAR-T cell manufacturing.
2. Monocyte Depletion
3. T-Cell Activation
4: Lentiviral Transduction
5: CAR-T Cell Production
6: Expansion to Target Dose
7: Formulation & Cryopreservation
Why NexCAR19™ ?
NexCAR19™ demonstrates strong clinical efficacy with rapid response rates, durable remissions, and a streamlined manufacturing timeline – addressing critical unmet needs in relapsed/refractory B-cell malignancies.
Safety & Efficacy Highlights
B-ALL
73% Complete Response Rate in Adult & Adolescent
1 Year PFS with BM Blasts < 25%
1 Year OS with BM Blasts < 25%
B-NHL
72% Overall Response Rate
1 Year PFS with MB Volume < 100 cubic cm
1 Year OS with MB Volume < 100 cubic cm
Treatment Process
Publications
Read our publications, published in prestigious journals such as The Lancet Haematology, Molecular Cancer Therapeutics by AACR and Blood by the American Society of Hematology.
Novel humanized CD19-CAR-T (Now talicabtagene autoleucel, Tali-cel™) cells in relapsed/ refractory pediatric B-acute lymphoblastic leukemia- an open-label single-arm phase-I/Ib study
Article
Apr 24, 2025Talicabtagene Autoleucel for Relapsed or Refractory B-cell Malignancies: Results from an Open-label, Multicentre, Phase 1/2 Study
Article
Apr 1, 2025Excellent Safety Profile of a Low-Cost Novel Humanized CD19 CAR T-Cell Therapy, Actalycabtagene Autoleucel : Potential Impact on Access and Feasibility
Abstract
Dec 9, 2023
NexCAR19™ Prescribing Information Guide
Essential prescribing information and medication guide for NexCAR19™ (Acetalycabtagene autoleucel), a CAR-T cell therapy for treating relapsed/refractory B-cell lymphomas and B-cell acute lymphoblastic leukemia. Includes detailed dosing instructions, safety information, and patient counseling guidelines.
Partnered Hospitals
Our strong association with over 80 leading cancer treatment hospitals in India ensures hassle-free treatment with our CAR-T cell therapies.
